TAPVR in the NICU
Total Anomalous Pulmonary Venous Return (TAPVR) in the NICU: Presentation, Management, and Nursing Considerations
Congenital heart disease is one of those areas of NICU practice where the physiology really matters at the bedside. Understanding why a baby is doing what they're doing helps you anticipate changes, escalate early, and advocate confidently for your patient.
Total Anomalous Pulmonary Venous Return (TAPVR) is one of those conditions you need to understand and have in the back of your mind. It's not the most common CHD you'll see, but when it presents, it can be dramatic, and it moves fast. It also could easily show up on the RNC-NIC and CCRN-N exams, so let's break it down.
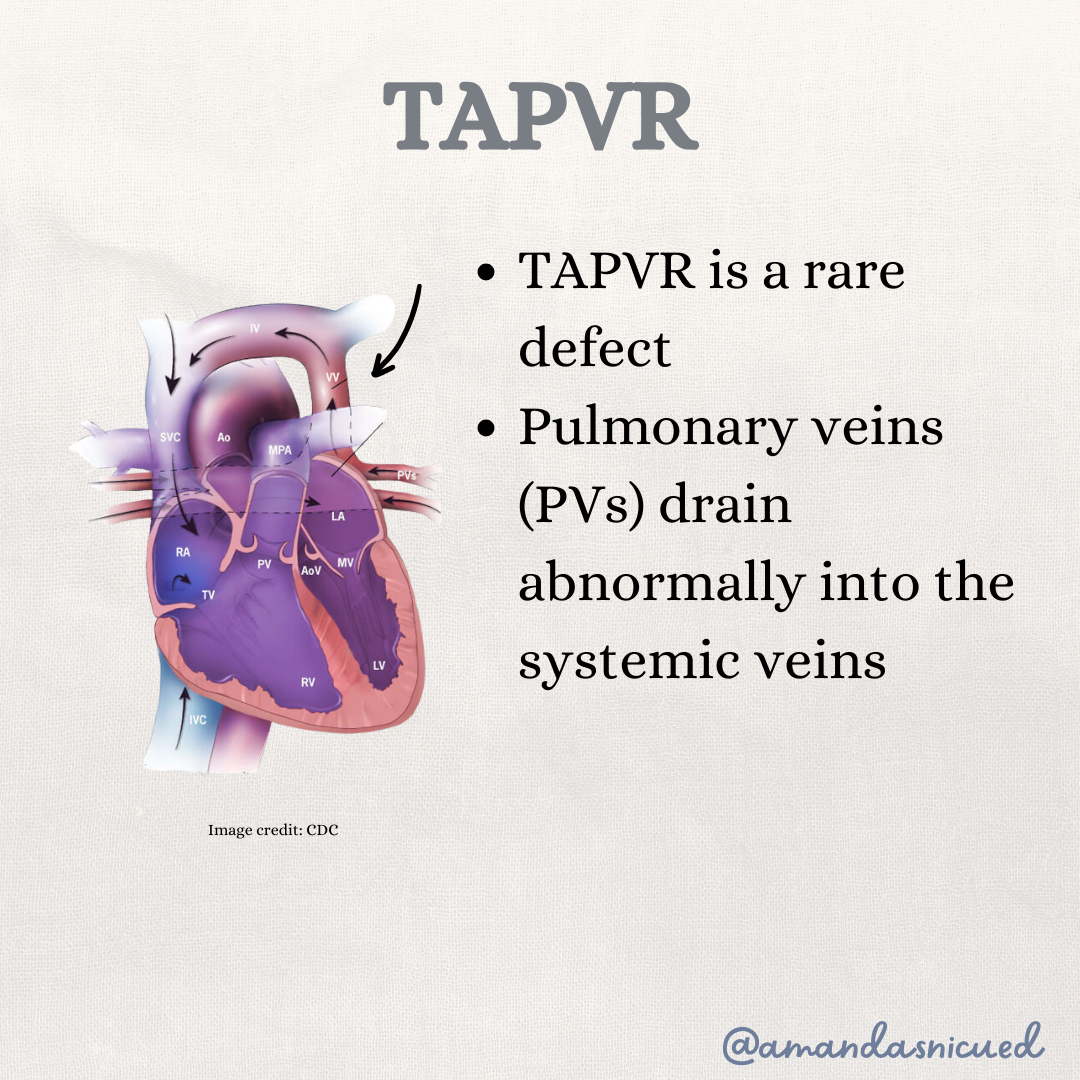
What Is TAPVR?
In a normal heart, the pulmonary veins return oxygenated blood from the lungs directly to the left atrium, where it heads out to the body. In TAPVR, that connection forms incorrectly during fetal development. Instead of draining into the left atrium, the pulmonary veins connect to the systemic venous circulation. This causes oxygenated blood to return to the right side of the heart instead of the left atrium.
What does that mean clinically? Oxygenated and deoxygenated blood mix together in the right side of the heart. For any of that blood to reach the left heart and get out to the body, it has to cross through an atrial septal defect (ASD). That ASD is the only reason these babies survive until surgery.
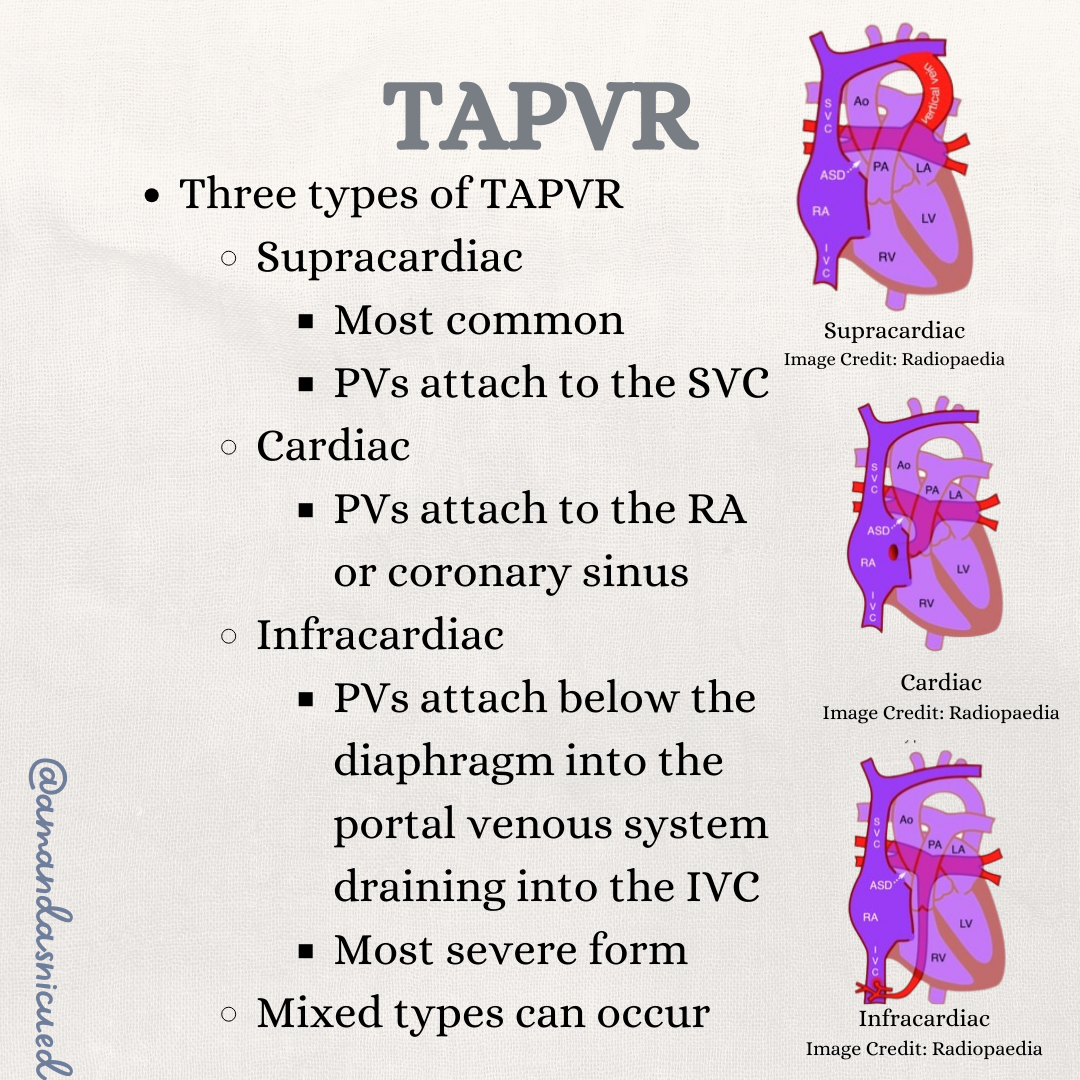
The Four Types
TAPVR is classified by where the abnormal drainage goes:
Supracardiac (most common): Pulmonary veins drain upward, typically into the superior vena cava via a vertical vein
Cardiac: Pulmonary veins connect directly to the right atrium or coronary sinus
Infracardiac: Pulmonary veins drain below the diaphragm, often into the portal venous system.
This type has the highest risk of obstruction
Mixed: Multiple abnormal drainage pathways, the least common form.
The type matters clinically because some are far more likely to become obstructed.
How These Babies Present
This is where your assessment skills are critical, because TAPVR doesn't always look the same.
Unobstructed TAPVR may be subtle at first. These babies can look deceptively stable: mildly cyanotic, mildly tachypneic. Gradually they develop signs of pulmonary overcirculation and heart failure. You might notice poor feeding, hepatomegaly, and oxygen saturations that are low but don't respond much when you increase FiO2.
Obstructed TAPVR is a different story entirely. This is a neonatal emergency. These infants often present within hours of birth with severe cyanosis, respiratory distress, grunting, and metabolic acidosis. Their chest X-ray frequently shows pulmonary edema and diffuse haziness; a picture that can look a lot like respiratory distress syndrome at first glance. If a baby looks critically ill and is not responding to oxygen or respiratory support, TAPVR needs to be on your differential.
RNC & CCRN Study Tip: Prostaglandin E1 generally does not improve oxygenation in TAPVR because systemic blood flow depends on atrial-level mixing rather than ductal flow. The ASD is the mixing point, not the ductus arteriosus.
Causes and Pathophysiology
TAPVR occurs because of abnormal embryologic development in the pulmonary venous system. Normally, a common pulmonary vein develops and connects to the left atrium, with individual pulmonary veins branching off it. In TAPVR, that connection fails to form, and the pulmonary veins instead find their way to systemic venous structures.
Infants with TAPVR require an atrial-level shunt (ASD or PFO) so oxygenated blood can reach the left side of the heart and be pumped to the body.. The downstream consequences of TAPVR are significant. The right heart becomes volume overloaded. Pulmonary circulation gets congested. And because oxygenated blood is being redirected away from the left heart, systemic oxygen delivery drops. When obstruction is present, pulmonary venous pressure rises sharply, leading to pulmonary edema and severe hypoxia.
Diagnosis and Initial NICU Management
TAPVR is diagnosed on Echocardiogram, cardiac CT angiogram, or cardiac catheterization but you may notice certain findings in your clinical assessment:
No Obstruction (typical has minimal symptoms):
PMI at the xiphoid process or Left lower sternal border
S2 widely split- pulmonic sounds may be pronounced
Mild-Moderate cardiomegaly with increased pulmonary markings on CXR
Characteristic "snowman sign" due to left SVC and innominate vein (rarely visible prior to ~4 months of age)
ECG: peaked p waves and RV hypertrophy
Right heart failure will develop over time
In unobstructed TAPVR with an unrestrictive ASD, cyanosis is usually mild and complete repair can wait until 3 to 6 months of age.
Obstructed TAPVR
Single loud S2
Gallop rhythm
Severe cyanosis, unresponsive to increased oxygen administration
Normal heart size with signs of pulmonary edema
Cardiogenic Shock
Your role is stabilization and close monitoring while the surgical team prepares for repair.
Initial support typically includes respiratory support (e.g. intubation), oxygen therapy, and correction of metabolic acidosis. Hemodynamic monitoring is essential. Oftentimes, the team may initiate inotropic support for poor cardiac output, diuretics for pulmonary congestion, and careful fluid management to avoid worsening the situation. Infants with severe obstructed TAPVR may require ECMO for stabilization prior to surgical repair.
As the bedside nurse, you're watching perfusion, urine output, respiratory status, and how the baby is responding to every intervention. These are the babies where your clinical instincts and early escalation can genuinely change outcomes.
Definitive treatment is surgical repair by connecting the pulmonary veins to the left atrium and closing the ASD. Obstructed TAPVR requires emergent surgery.
Post-Op Complications to Watch For
After surgical repair, common complications you'll monitor for include:
Pulmonary hypertension
Low cardiac output syndrome
Arrhythmias
Pulmonary vein stenosis (a serious concern, particularly in infracardiac TAPVR)
Residual pulmonary edema
Post-op management often involves mechanical ventilation, vasoactive medications, and meticulous fluid balance.
Outcomes
With advances in neonatal cardiac surgery and post-operative care, outcomes for TAPVR have improved considerably. Prognosis is influenced by whether obstruction was present, how quickly the diagnosis was made, whether associated anomalies exist, and how the post-op course goes. Many infants who undergo timely repair go on to do well, though long-term cardiology follow-up is always needed.
Key Takeaways for NICU Nurses
Oxygen-resistant cyanosis + pulmonary edema should put TAPVR on your radar
An ASD is essential for survival
Prostaglandin E1 is not the answer in TAPVR
Obstructed TAPVR is a neonatal emergency requiring emergent surgery
Early recognition and stabilization are your most powerful tools
Ready to Feel More Confident with NICU Cardiac Conditions?
CHD can feel overwhelming — especially when you're trying to keep the physiology straight while also preparing for certification. Inside my NICU Certification Review Course, I break down complex topics like TAPVR, neonatal shock, and congenital heart defects into clear, exam-ready lessons built specifically for NICU nurses.
✔ Hundreds of nurses have already passed their certification using this course ✔ High-yield content explained in a way that actually makes sense ✔ Practice questions to reinforce the concepts
👉 Learn more about the NICU Certification Course here.
References
Johnson, G., & Goff, D. (2027). Cardiovascular system. In K. Kenner, L. Altimier, & M. Boykova (Eds.), Comprehensive neonatal nursing care (7th ed.). Springer Publishing.
Swanson, T., & Erickson, L. (2026). Cardiovascular diseases and surgical interventions. In D. Enzman-Hines, B. Carter, & S. Niermeyer (Eds.), Merenstein & Gardner's handbook of neonatal intensive care. Elsevier.
Gonzalez-Estevez, N., & Anash, D. (2024). Congenital heart disease. In J. Gleason & T. Sawyer (Eds.), Avery’s diseases of the newborn. Elsevier.
Bocks, M., Boe, B., & Wilder, T. (2025). Neonatal management of congenital heart disease. In R. Martin & A. Fanaroff (Eds.), Fanaroff and Martin’s neonatal-perinatal medicine. Elsevier.
