
3 Disorders Every NICU Nurse Should Know
Newborn Screening in the NICU: 3 Disorders Every Nurse Should Understand
Newborn screening is one of the most powerful tools we have in neonatal care and yet it's one of the areas where bedside nurses sometimes feel least confident.
That makes sense. The results come back, they flag something, and suddenly there's a flurry of activity: repeat labs, phone calls to metabolic teams, anxious families. If you don't understand the why behind what's happening, it's easy to feel like you're just watching from the sidelines.
You are not a bystander in this process. You are often the first person to notice that something isn't quite right with the baby. You're the one collecting the specimen, monitoring for early signs, and advocating for the infant when results seem off. That's why understanding these conditions at a deeper level matters so much, both at the bedside and on your certification exam.
Let's walk through three high-yield disorders that every NICU nurse should truly understand:
Congenital hypothyroidism (CH)
Phenylketonuria (PKU)
Galactosemia
Congenital Hypothyroidism (CH):
The physiology
Thyroid hormone (specifically the conversion of T4 to its active form T3) is essential for brain development, growth, metabolism, and thermoregulation. In the first hours after birth, newborns experience a TSH surge followed by a rise in both T4 and T3 over the next 24–36 hours. This normal postnatal transition is important to understand, because it directly impacts when we screen and how we interpret results.
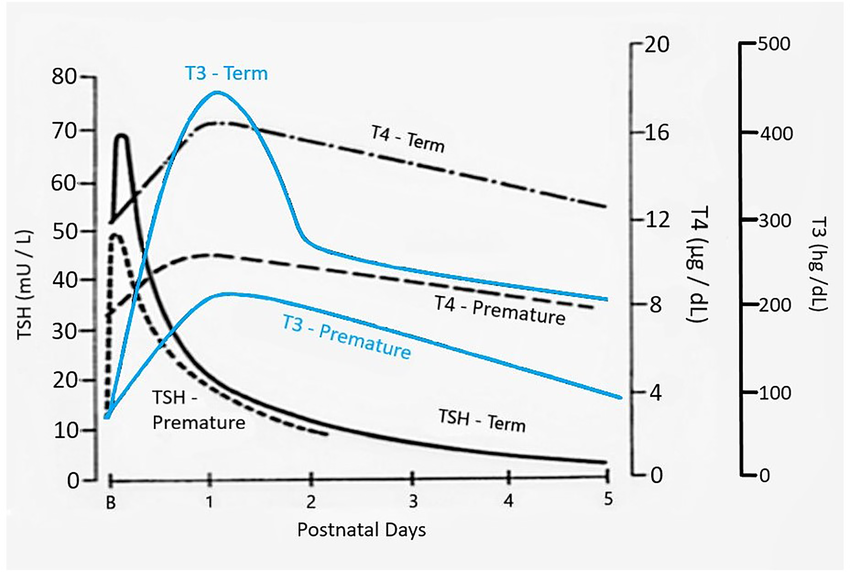
LaFranchi SH (2021)
What goes wrong
Congenital hypothyroidism occurs when there is insufficient thyroid hormone production. The most common reason is thyroid dysgenesis: meaning the thyroid gland is absent, underdeveloped, or in the wrong location. It's one of the most common preventable causes of intellectual disability, affecting roughly 1 in 2,000 to 4,000 newborns worldwide.
Clinical presentation
Most infants with CH have no signs at birth. Why? Because maternal thyroid hormone crosses the placenta and temporarily compensates for the baby's deficit. As those maternal levels decline in the days following delivery, symptoms begin to emerge. You might start to see:
Lethargy and poor feeding
Hypotonia ("floppy" muscle tone)
Hypothermia
Prolonged jaundice
By the time these signs are obvious, the window for preventing neurodevelopmental harm is narrowing.
In the NICU…
This is where it gets nuanced for us. In the NICU,illness and certain medications like dopamine and corticosteroids can suppress thyroid function and distort results. Preterm infants, very low birthweight neonates, and infants admitted to the NICU who have a normal first screen still warrant a second screening at 2 to 4 weeks of age. For premature infants, if that second screen is also normal, guidelines recommend repeat testing again four weeks later. The delayed TSH rise that can occur in preterm infants means a single normal result early in the hospital course is not sufficient reassurance. One study of NICU infants with delayed TSH rise found that 58% ultimately required levothyroxine treatment. Showing us just how important that repeat screen is.
Bottom line: Many NICU babies require repeat screening. Does your NICU repeat newborn screens or thyroid testing?
Treatment
Prompt diagnosis through newborn screening, leading to early and adequate treatment, results in grossly normal neurocognitive outcomes in adulthood. The standard initial treatment is levothyroxine, at 10 to 15 mcg/kg daily, with the goal of maintaining normal TSH and free T4 levels. Treatment should begin within 1 to 2 weeks of life. Early intervention is brain protection.
Phenylketonuria (PKU):
The physiology
PKU is an autosomal recessive disorder of amino acid metabolism. Affected infants lack a functioning phenylalanine hydroxylase (PAH) enzyme, which means they cannot convert phenylalanine into tyrosine. This results in the accumulation of phenylalanine and related metabolites, which can negatively impact growth and neurodevelopmental outcomes, particularly in infants and children.
The more protein the baby takes in (whether from breastmilk, formula, or TPN) the more phenylalanine builds up in the bloodstream, silently doing damage to the developing brain.
Clinical presentation
Most infants with PKU have no signs at birth. That's exactly why screening exists. If PKU is missed (or if feeding history creates a false result and the diagnosis is delayed) you may eventually see:
Poor feeding and irritability
Vomiting
A musty or "mousy" body odor (a distinctive clinical clue)
Eventual developmental delay
The symptoms of untreated PKU develop gradually, so they may not be noticed until irreversible intellectual disability has already occurred.
In the NICU…
PKU screening is directly tied to protein exposure, and this creates two distinct problems for NICU patients:
False negatives: If an infant hasn't received adequate protein (feeds haven't started, or are minimal), phenylalanine levels won't have built up enough to trigger the screening threshold. The result looks normal, but it's not a reliable result.
False positives: On the flip side, TPN, which supplies amino acids, and the liver immaturity of preterm infants are recognized as major contributors to high false-positive newborn screening rates in the NICU. An elevated phenylalanine on screening in a TPN-dependent infant may reflect the amino acid load rather than a true inborn error of metabolism.
Some NICUs have implemented evidence-based protocols to address this: one intervention involved replacing TPN with a dextrose infusion for 3 hours before specimen collection, which significantly reduced false-positive results.
As the bedside nurse, knowing the infant's feeding and nutrition history at the time of specimen collection is essential context for interpreting the result.
Treatment
With early detection and implementation of a phenylalanine-restricted diet, intellectual development is substantially better than when the disorder is diagnosed years later. Treatment involves a low-phenylalanine diet, specialized metabolic formula, and lifelong management with metabolic specialist oversight.
Galactosemia:
The physiology
Galactosemia is a disorder of carbohydrate metabolism. In classic galactosemia, a deficiency of the enzyme galactose-1-phosphate uridylyltransferase (GALT) means the infant cannot properly convert galactose into glucose. Within days of ingesting breastmilk or lactose-containing formulas, infants with classic galactosemia can develop life-threatening complications including feeding problems, failure to thrive, hypoglycemia, hepatocellular damage, bleeding, and jaundice.
Unlike CH and PKU (which are silent early) galactosemia announces itself quickly once feeding begins.
Galactosemia and E. Coli
A term newborn presenting with E. coli sepsis in the first days of life should raise immediate suspicion for galactosemia. Why? Because galactosemia patients are particularly susceptible to E. coli infection, which can evolve into neonatal sepsis. Sepsis may actually precede the formal diagnosis of galactosemia. The accumulation of galactose metabolites appears to impair the infant's immune defenses, making them exquisitely vulnerable to gram-negative organisms.
In the NICU…
Signs of galactosemia can appear before newborn screening results are back. The standard turnaround time for newborn screening is several days, and a galactosemic infant who has been breastfeeding or receiving lactose-containing formula since birth may already be in crisis by then.
If galactosemia is clinically suspected the infant should be immediately placed on a lactose-restricted diet.
Treatment
The intervention is a lactose-free diet and when provided during the first three to ten days of life, the signs of classic galactosemia resolve quickly, and the prognosis for prevention of liver failure, E. coli sepsis, and neonatal death is significantly reduced.
That means:
No breastmilk
No standard formula
Start lactose-free, soy-based formula immediately
Putting It All Together: What NICU Nurses Need to Know
These three disorders highlight something fundamental about newborn screening: not all conditions behave the same way, and not all timelines are equal.
As a NICU nurse, your role is imperative:
Understanding how physiology impacts screening results (so you know when a result may be unreliable)
Knowing when to advocate for a repeat screen (especially in premature or critically ill infants)
Recognizing early signs of metabolic decompensation before the lab calls you
Knowing when a diagnosis like galactosemia requires you to act and how
For Nurses Preparing for Certification
Congenital hypothyroidism, PKU, and galactosemia are high-yield topics for both the RNC-NIC and CCRN-N exams. You can expect questions about their pathophysiology, clinical presentation, NICU-specific screening nuances, and treatment priorities. More importantly, they are conditions where your depth of understanding translates directly into better outcomes at the bedside.
References
LaFranchi SH (2021) Thyroid Function in Preterm/Low Birth Weight Infants: Impact on Diagnosis and Management of Thyroid Dysfunction. Front. Endocrinol. 12:666207. doi: 10.3389/fendo.2021.666207
Rose SR, Wassner AJ, Wintergerst KA, et al; Section on Endocrinology Executive Committee, Council on Genetics Executive Committee. Congenital hypothyroidism: screening and management. Pediatrics. 2023;151(1):e2022060420. https://doi.org/10.1542/peds.2022-060420
Léger J, Olivieri A, Donaldson M, et al; ESPE-PES-SLEP-JSPE-APEG-APPES-ISPAE Congenital Hypothyroidism Consensus Conference Group. European Society for Paediatric Endocrinology consensus guidelines on screening, diagnosis, and management of congenital hypothyroidism. J Clin Endocrinol Metab. 2014;99(2):363–384. https://doi.org/10.1210/jc.2013-1891
Shayota BJ, Rose N. Phenylketonuria (PKU): Primary care guide to a positive newborn screen. Topical Reviews in Pediatrics. Updated November 2024. https://trip.utah.edu/phenylketonuria-pku-primary-care-guide-to-a-positive-newborn-screen/
Stewart J, Allen H, Birnbaum A, et al. Pausing TPN to decrease abnormal newborn screens: a NICU quality initiative. BMC Pediatrics. 2021. https://pmc.ncbi.nlm.nih.gov/articles/PMC8475792/
Berry GT. Classic galactosemia and clinical variant galactosemia. In: Adam MP, et al., eds. GeneReviews. Seattle, WA: University of Washington; updated 2021. https://www.ncbi.nlm.nih.gov/books/NBK1518/
Badiu Tișa I, Achim AC, Cozma-Petruț A, et al. The importance of neonatal screening for galactosemia. Nutrients. 2022;15(1):10. https://doi.org/10.3390/nu15010010
Berry GT. Galactosemia: when is it a newborn screening emergency? Mol Genet Metab. 2012;106(1):7–11.
American College of Medical Genetics. Classical galactosemia (GALT) ACT sheet. Updated 2024. https://www.dshs.texas.gov/sites/default/files/newborn/pdf/ActGalt.pdf
HRSA Newborn Screening. Classic galactosemia. https://newbornscreening.hrsa.gov/conditions/classic-galactosemia
